Mom's Plastic Brain: A Story in 3 Parts
How the Science of Neuroplasticity Convinced Me to Fake it Until I Made it

Author’s Note: I’ve written generally about my disability many times, but I’ve never told the whole story. In the course of 6 hours, I went from being an “young, active mom” with a career in education to a “35yo left handed f” presenting with left-sided hemi-paresis (paralysis). This is part one of my story. I’ll release parts two and three over the next month.
Part One: Away
The first time I learned about neuroplasticity, the brain’s ability to rewire itself in response to a new experience, injury, or trauma, I was in graduate school studying to become a teacher. We learned that our students’ malleable brains thirst for new experiences in order to expand neural pathways. We read about songbirds whose brains quickly rewire to change their tune by season. We watched videos of three-year-olds skillfully playing Mozart thanks to the Suzuki method of violin instruction. I was fascinated by the concept that our brains are more capable of change than scientists once believed. In my thirteen years teaching high school English, I would apply this knowledge by inviting my students to engage deeply with a wide variety of literature, film, journalism, advertising and poetry. Small group discussions and open ended questions gave students’ brains the new perspectives they craved.
So it took me by surprise when I learned about neuroplasticity all over again from a hospital bed on the stroke-care unit of a rehabilitation hospital. On the first night of a family vacation, a sudden, catastrophic, and “stroke-mimicking” flare of my normally docile Multiple Sclerosis had rendered my entire left side paralyzed, shoulder to toes. I would remain hospitalized for a month, leaving my spouse Peter to care for our children, four year old Paul and six year old Marie. During daily rounds, an anonymous physician would lift my heavy limp left arm and struggle to place my hand just right, so that four of my fingers rested upon one of their smooth, gloved fingers. They’d ask me to squeeze as hard as I could, and we would both stare as my fingers, clearly not moving a muscle, slipped downward from the weight of gravity. Through tears I’d say, “I’m squeezing as hard as I can!” and clutch the clean cotton hospital blanket with my right hand, overtaken by uncontrollable sobs. I learned later that the uncharacteristic crying jags and the paralysis of my left side were connected. A 38 millimeter necrotizing lesion called a “black hole” (their words not mine) in my right brain had essentially destroyed all tissue in the “motor strip,” hence the left sided paralysis, or weakness, as doctors liked to call it. The Apple Watch face-sized hole had brushed up against my right frontal lobe - the part that controls our ability to regulate emotions. When I cried, I would heave and have trouble getting breath; the slightest bit of humor would send me into laughter so hard my stomach hurt, badly. This condition is called pseudo-bulbar affect (PBA), or emotional incontinence, and luckily my case lasted only a few months.
Becoming disabled in my thirties, midway through an able-bodied life, was shocking. I did not work in a medical adjacent field, nor had I intimately cared for a loved one, so I had not thought about the practicalities of maneuvering through the day as a disabled person. A numb understanding washed over me when I sat on a toilet, flanked on either side by medical assistants: “this is how I pee now.” I felt torn between gratefulness for the excellent care I was receiving, and horror at the fact that I needed care. Always, I was angry at myself for having taken previously “simple” tasks for granted. Sitting upright in bed, opening a can of ginger-ale, and putting up my graying chestnut hair had become two person activities. After a week of failing to accomplish a messy bun one-handed, my head felt unbearably off. After sending pixie undercut hairstyles to my friends for guidance, I settled on an angled bob and made an appointment from my hospital bed in preparation for my new normal. The fact that I could use a phone at all felt like a gift, an island of familiarity in the sea of chaos that accompanies brain injury. My phone was too unwieldy to hold in my non-dominant right hand, but thanks to a popsocket and dictation capability (both essential assistive technologies), I could connect with my children daily. Peter and I quickly realized that real-time “check-ins” with Mommy were doing more harm than good. Because of emotional incontinence, I was unable to control the cracking voice and streaming tears that began as soon as their excited smiles bobbed into view. Asynchronous video messages were a crucial replacement, and I took advantage of silly filters to hide my reddened face as I wished them good morning and kissed them goodnight.
My inpatient occupational therapist, a ferociously patient woman named Dana, told me she expected me to recover hand function at least partially, if not fully. Hearing this, I exploded with tears and wails, once again interrupting our session. I had been “pushing” a soft rag across a smooth table. Dana was doing the work, and my left arm was just along for the ride. I told Dana that I trusted her, but when she spoke of recovery, she may as well have been talking about literal magic. I couldn’t imagine a world in which my heavy yet floppy arm and hand moved on command, just as I had never imagined they could stop moving on command. Dana explained that thinking about my arm moving, imagining my arm pushing the cloth was my only goal for that session. Our goal was to move my bad arm (“not your bad arm, your affected arm! She’d correct me”) together. Passive movement, with her doing the work and me believing I was doing it, was the key to creating new neural pathways in place of those destroyed by MS. That night in the never quite dark hospital, I looked up articles about neuroplasticity, barely aware it was the same concept I’d learned so long ago.
“[Dr.] Doidge argues that brain-as-machine is an outdated metaphor because it misses our brains’ remarkable ability to adapt and repair damage by carving out new pathways with neural connections. “
My search led me to the 2008 documentary The Brain That Changes Itself, based on the eponymous book by neuroscientist Norman Doidge. Dr. Doidge explains that for hundreds of years, scientists viewed the brain as a complex machine with hard parts that perform one or two specific functions each. If a part was broken or lost, so too was its function. In the years that have followed, I’ve studied Doidge’s first text as well as the followup, The Brain’s Way of Healing. Doidge argues that brain-as-machine is an outdated metaphor because it misses our brains’ remarkable ability to adapt and repair damage by carving out new pathways with neural connections. The film follows Michelle Mack, born without a left hemisphere in her brain. We see an adult Michelle living independently and communicating clearly about the complexities of her life. Michelle’s story directly challenges mechanical brain theory, which holds that the left hemisphere is responsible for speech, comprehension, and analytical thinking. Clearly, Michelle’s right and only hemisphere have created the pathways necessary for these functions. Michelle’s family credits her dedication to trying repeatedly at left brain functions. As Dr. Doidge says, “mental activity is not only the product of the brain, but also a shaper of it.” So, imagining my arm pushing a rag could result in motor return. I felt confident in my potential for the first time since I’d been wheeled into the hospital on a stretcher.
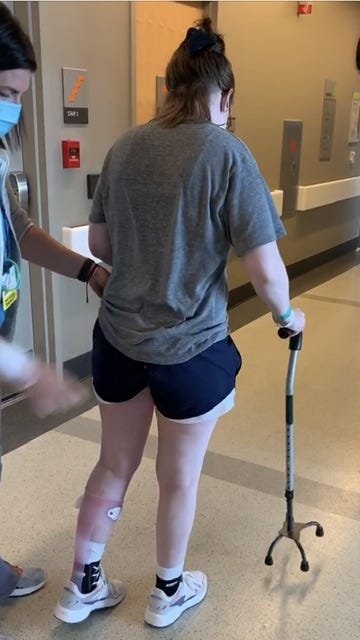
After a month, I was capable of walking 100 feet, heavily supported by a four-pronged cane and a heavy leg brace. I had successfully practiced getting into and out of a bath chair, and even washed dishes and chopped items with assistive cutting boards. I had passed a balance test, and was proud of accomplishing what only weeks ago had been simple tasks. The magic of neuroplasticity seemed to be humming right along with my left leg. But there was reason for concern. My left arm remained entirely paralyzed, shoulder to fingers, and the random, uncontrollable sobbing fits had subsided, but hadn’t stopped. Discharge day happened to fall on July 14, Bastille Day in France, and I imagined I was being liberated by my family, finally allowed into the world again. Every single therapist wished me well and warned me how much more work was in store once I was home. Their warnings were a reminder of how taxing it had been to wash and put away a single plastic tumbler - how out of breath and dizzy I’d felt at 100 feet of walking. But I was so happy to be going home to my kids that I felt only joyful anticipation on that 14 Juillet.
As Peter drove us home from the hospital, I was caught off-guard by waves of intense nausea. Apparently, I had developed a new and severe motion sickness in the hospital; an unwelcome surprise. There had been a hint, though. Holding my head in my right hand as the storefronts and signs swirled past, it occurred to me that I recognized this sick to my stomach, dizzy feeling: it was the exact feeling I had gotten when my care team would push me around the hospital in a wheelchair. I didn’t know then that the motion itself was making me nauseous, and of course in a car it was exponentially worse. For once, something about my situation made sense, even if it was painful. This realization was proof that my body had many answers, if only I would listen. Before my flare, I had a rewarding but intense time teaching in a public high school during the pandemic, while also (alongside my spouse) caring for my kids and our home. Add in the stress of washing groceries and no vaccine in sight, I hit some kind of maximum stress point. As a result, my body finally and literally stopped me in my tracks with paralysis. My body had been trying to speak to me for so long, but I had missed the signs. I thought it might be saying, “slow down, manage your stress, CHILL OUT ERIN.” In the years that followed, I would listen closely for clues from the body I’d ignored.
Erin Ryan Heyneman is a disabled educator, creator, and speaker. She is also a Commissioner on her city’s Commission on Disability. Find the rest of her work here





This is so moving and relatable, thank you for writing it. I will be thinking about the phrase "emotional incontinence" forever now :)